PERCUTANEOUS CORONARY INTERVENTION
Percutaneous coronary intervention began on-site on 18/6/1986. For several months preceeding this, Peter Leslie and Richard Thompson, accompanied by Wellington patients, had made trips to Dunedin to learn the technique from Drs Michael Ablett and Charles Illsley who already had considerable experience in the technique.
Until around 1994, numbers of percutaneous coronary angioplasties done were relatively low. In 1994, David Smyth performed the first coronary stent placement and from 1996, such procedures rapidly increased in number. Very soon, the number of PTCA's without stenting were relatively few.
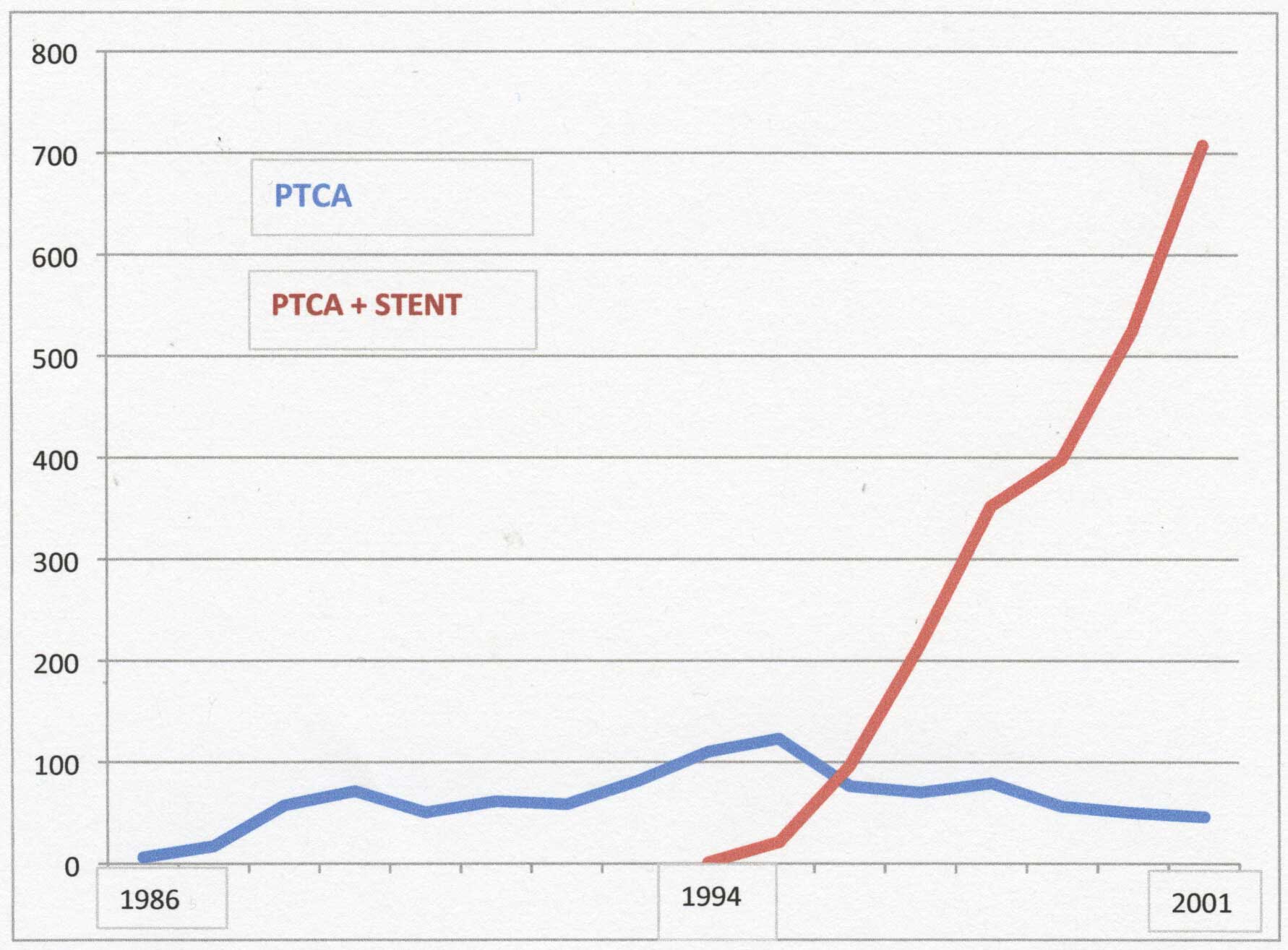
It took just over 11 years to complete the first 1,000 coronary interventions, a milestone celebrated by Peter Leslie and his team on 17/9/1997.
A little over two years later, the next 1,000 coronary interventions were completed (6/1/2000).
Percutaneous coronary interventions have been performed at an average rate of 873/year over the years 2004 - 2011, and an average of 96% of these have included the placement of at least one stent. The majority of PCIs are done at the diagnostic procedure.
Percutaneous intervention for acute coronary disease is dealt with under Acute Coronary Syndromes.
PERCUTANEOUS AORTIC VALVULOPLASTY
Aortic valvuloplasty was first done by Richard Thompson in 1987 and was undertaken on 3 - 11 patients annually to 1994. Richard had departed for Wakefield Hospital in 1992 and enthusiasm for the procedure fell away with none being done after 1994 until more recently. Now, the balloon catheters are of improved design including the fact that the catheter size is smaller (9F). Currently such procedures are done by Mark Simmonds, Phil Matsis and Scott Harding.
Both Mark and Scott have gained training in the procedure of percutaneous aortic valve replacement, but funding has yet to be granted for this type of treatment in selected elderly, high surgical risk patients.
PERCUTANEOUS PULMONARY VALVULOPLASTY
A few pulmonary valvuloplasties were undertaken between 1987 and 1994 (6 patients in all), but since that time any patients with pulmonary stenosis have been referred to Auckland for such treatment.
PERCUTANEOUS MITRAL VALVULOPLASTY
Richard Thompson performed a single mitral valvuloplasty in 1991 as did David Smyth in 1994. Phil Matsis began a more regular programme in 1998 and by the end of 2001 had undertaken 31 procedures.
Currently Phil does an average of 10 procedures annually. The referral base extends from Taranaki and Hawkes Bay to the north and Nelson and Christchurch to the south.
A key advance has been improved echocardiography assessment and Phil acknowledges the skills of Alex Sasse here. Recently, 3-D echo has helped by giving a 'surgical' view of the stenosed valve.
Surgical mitral valvotomies are no longer performed.
PERCUTANEOUS CLOSURE OF PFO AND ASD
Alex Sasse and Phil Matsis have run this programme in the past few years.
In regard to closure of PFOs, the patients are typically younger stroke patients who show evidence of a PFO with echocardiography bubble studies. Around 50 such patients have had their PFOs occluded percutaneously.
A smaller number of patients with ASDs have also had successful percuatneous occlusion of their lesions.