There has been considerable evolution in the use of radiographic investigations since the cardiology service was first established. Some of the changes that have taken place are dealt with here.
(Cardiac angiography is dealt with under Cardiac Catheterisation(
The Chest X-Ray and other plain films
In the Cardiology OP Clinic in the 1960s and 1970s, it would be routine to order an ECG and CXR on all new referrals, and the results of these tests were available to the cardiologist when the patient was first seen. Similar routines were followed for follow-up patients.
It was David McHaffie who, in the 1980s, questioned this practice as he considered that the routine CXR did not usually contribute to the understanding of the patient's condition. Eventually the routine CXR became less-often performed but was requested when there seemed to be a specific question to answer. Once 2-D echocardiography became available it quite quickly replaced the CXR as a tool for understanding both structure and function in valvular, myocardial and congenital heart disease, although it remained useful for assessing pulmonary vasculature.
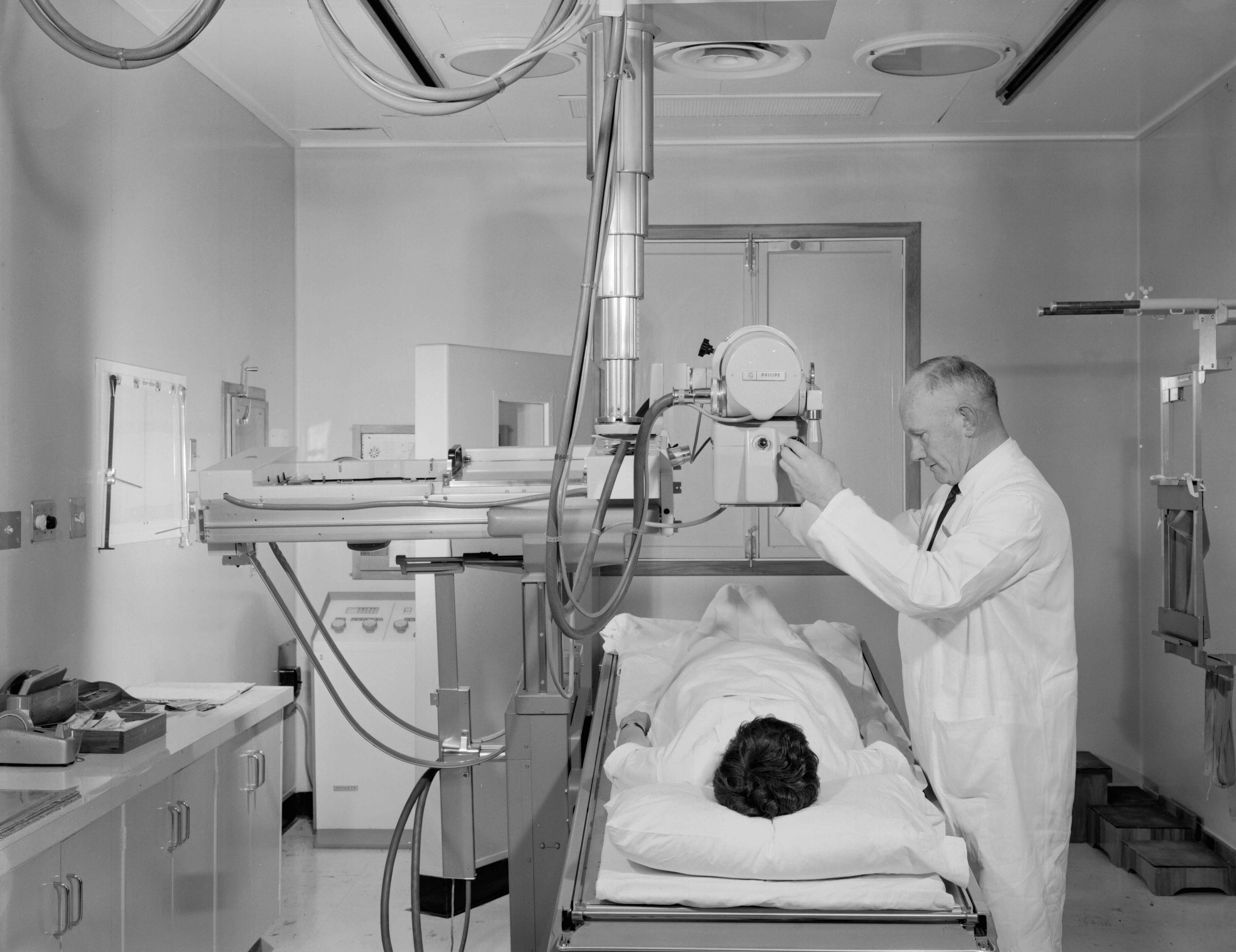
Plain xrays were quite often requested for cardiology inpatients. Adjacent to the Seddon Cath Lab was a small radiographic room where chest xrays and other plain films could be taken on patients from ward 22.
Here Ted Spiers readies a patient for a plain film.
Chest Screening
Radiographic screening of the chest accompanied by a barium swallow for the assessment of cardiac patients had been popularised in the 1930s by Sir John Parkinson in London.
Sir Charles Burns recalled "as regards the extent of investigation of patients with circulatory problems, it was our practice ... to have an electrocardiogram obtained and the heart screened." Burns thought that screening was better than the plain chest xray.
Reporting to the Wellington Hospital House Committee on 2/12/1954, Medical Superintendent Richard Durand wrote
"at present when the physicians want to screen a patient's heart they have to call on the X-ray Department. This takes up time in the X-ray Department and involves a good deal of wastage of manpower both for porters, visiting staff, radiologists and nurses. It is quite unneccessary for a radiologist to be present, or indeed a technician, for all physicians with experience in cardiology are trained and are as expert if not more expert in the interpretation of heart shadows than a radiologist."
This strong statement followed a bid by Charles Burns and John Keeling for the establishment of an x-ray screening unit within the cardiology department.
Needless to say, a response from the X-ray Department followed.
On 22.12.54 Dr Feltham, radiologist wrote
"In my opinion it would be a retrograde step if the Board permitted the purchase and the use of screening equipment in the Cardiology Department."
There followed a considerable correspondence from both sides but eventually, the case for a separate heart screening unit in the Cardiology Department won out, so that when the new department opened in 1958, a designated screening room was included.
In 1965, as a cardiology registrar, I participated in what may well have been the last chest screening procedure done in the Cardiology Department. I recall well that my job was to mix up and administer the barium paste to a patient of Marshall Luke. I can also admit that I never did become expert at interpreting the images resulting from the barium filled oesophagus running alongside the heart chanbers. By that time, the practice of routine chest screening had ceased.
Cardiac Magnetic Resonance Imaging
A Cardiac MRI service was established at Wellington Hospital in 2010. Prior to that, patients requiring a CMRI were referred to Hutt Hospital (where a service has been in operation since 2006), and before that, to Auckland Hospital.
Kathy Ferrier pioneered the service at Hutt Hospital and, with Alex Sasse, manages the service at Wellington Hospital.
On average, five patients are scanned each week in Wellington.
The key advantages of CMR over other imaging modalities are image quality, non-invasiveness, accuracy, versatility and the lack of ionising radiation. The key disadvantages are its limited availability and expense.
The images taken during MRI are for the most part gated-images acquired over 10-20 heartbeats. This means that image quality is degraded if there is arrhythmia although tachycardia with a regular rhythm is fine and rate-controlled AF usually doesn't degrade images too much. For each image the patient is required to hold their breath, usually for 10-20 seconds.
A basic scan assessing LV function takes 15-20 minutes but scans for complex congenital disease may take around an hour. Children as young as 10 years have been scanned without anaesthetic.
A common indication for CMR is the assessment of cardiomyopathy, both ischaemic and non-ischaemic. Visualisation of scar can aid with identifying aetiology, assessing viability of the tissue and providing risk assessment. The presence and degree of scarring are independent predictors of sudden cardiac death. This is particularly relevant if an ICD is being considered.
CMR is widely used to assess congenital heart disease, because of its ability to visualise the right heart and great vessels. When used in concert with echocardiography, the need for invasive assessment has been significantly reduced.
CMR is particularly valuable for older children and adults with congenital heart disease, in complex pathology, and after surgery when echocardiography may be difficult.
CMR is now commonly used to visualise the aorta. Whilst exam time is longer than with CT, it does not require intravenous contrast and does not involve ionising radiation. Thus CMR is now the modality of choice in younger patients and those with connective tissue diseases who may need multiple scans in their lifetimes.
I am grateful to Kathy Ferrier for the information on CMR.