Mark Hoby departed Wellington for Adelaide in 1985, and in 1986 Drs Vaughan Richardson and David Brabyn were appointed as neonatologists.
At that time there were eight ventilated infants, and six working monitors. Lani Wills oversaw 24 FTE nurses, and typically one nurse cared for three ventilated infants. The unit was overcrowded, there was no training course for neonatal nurses, and there was no biomedical technician on site in the unit. It was quickly established that more nurses were needed, a training course for nurses should be established, better equipment with a dedicated biomedical technician on site were required, and an improved unit layout. Increased RMO numbers were also needed.
By 1988, a Neonatal Nurses Training Course was established, coordinated by Rosemary Escott. Approval was given for twelve more full-time nurses immediately, with further increases to come.
A dedicated biomedical technician was based in NICU. Over $500,000 was spent on new equipment.
NICU registrars were augmented by SHO's and the registrars were able to remain in Wellington longer for training.
The physical size of the unit was increased in 1995 by adding wasted corridor space and joining the "back rooms".
 Rosemary Escott in Room 4 in 1996
Rosemary Escott in Room 4 in 1996
Space for babies, staff and equipment remained limited
Further space was added in 1998-1999 by converting the equipment room to ICU bed spaces and opening up the little-used "isolation rooms" to allow more distance between babies.
 Vaughan Richardson (left), Dawn Elder (right) and team
Vaughan Richardson (left), Dawn Elder (right) and team
Planning for the new Regional Hospital saw several options for a new NICU, the final one selected had the unit colocated with the Delivery Suite on Level 4. This allowed for expansion on to the roof space. The result was the well-designed unit that is in operation today.
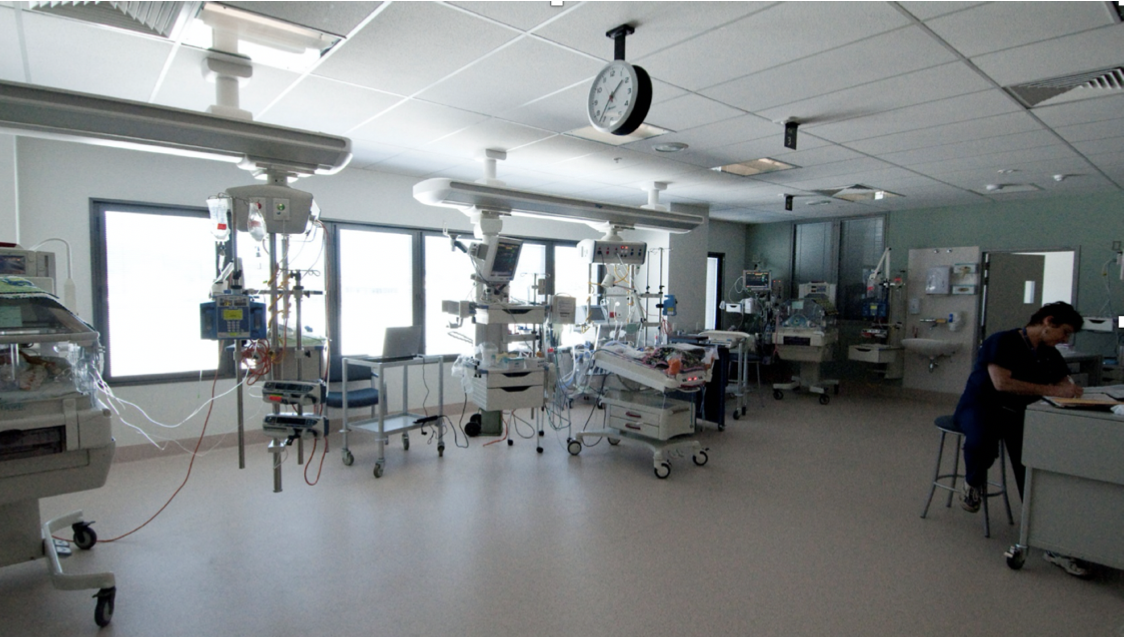
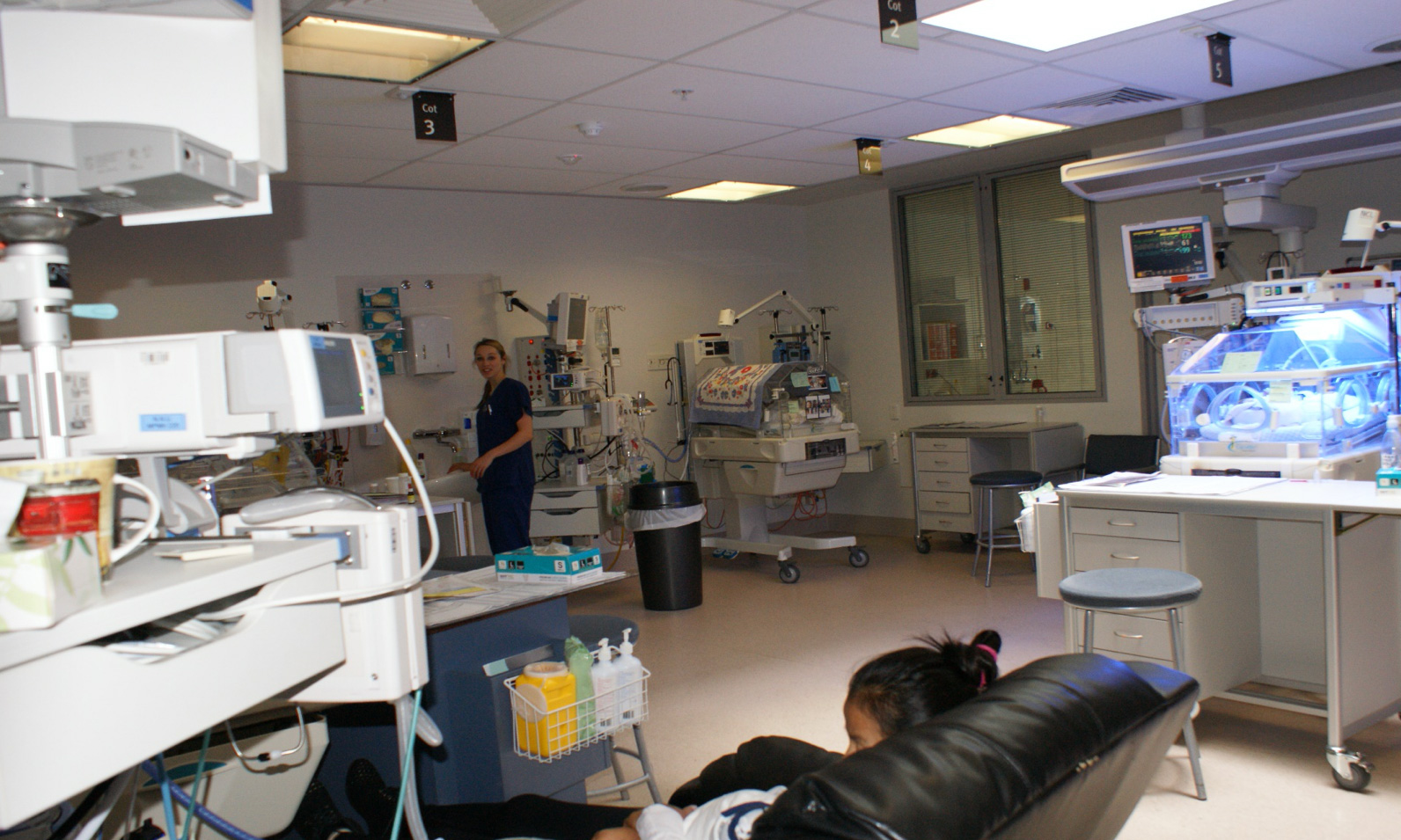 The new NICU - much more space
The new NICU - much more space
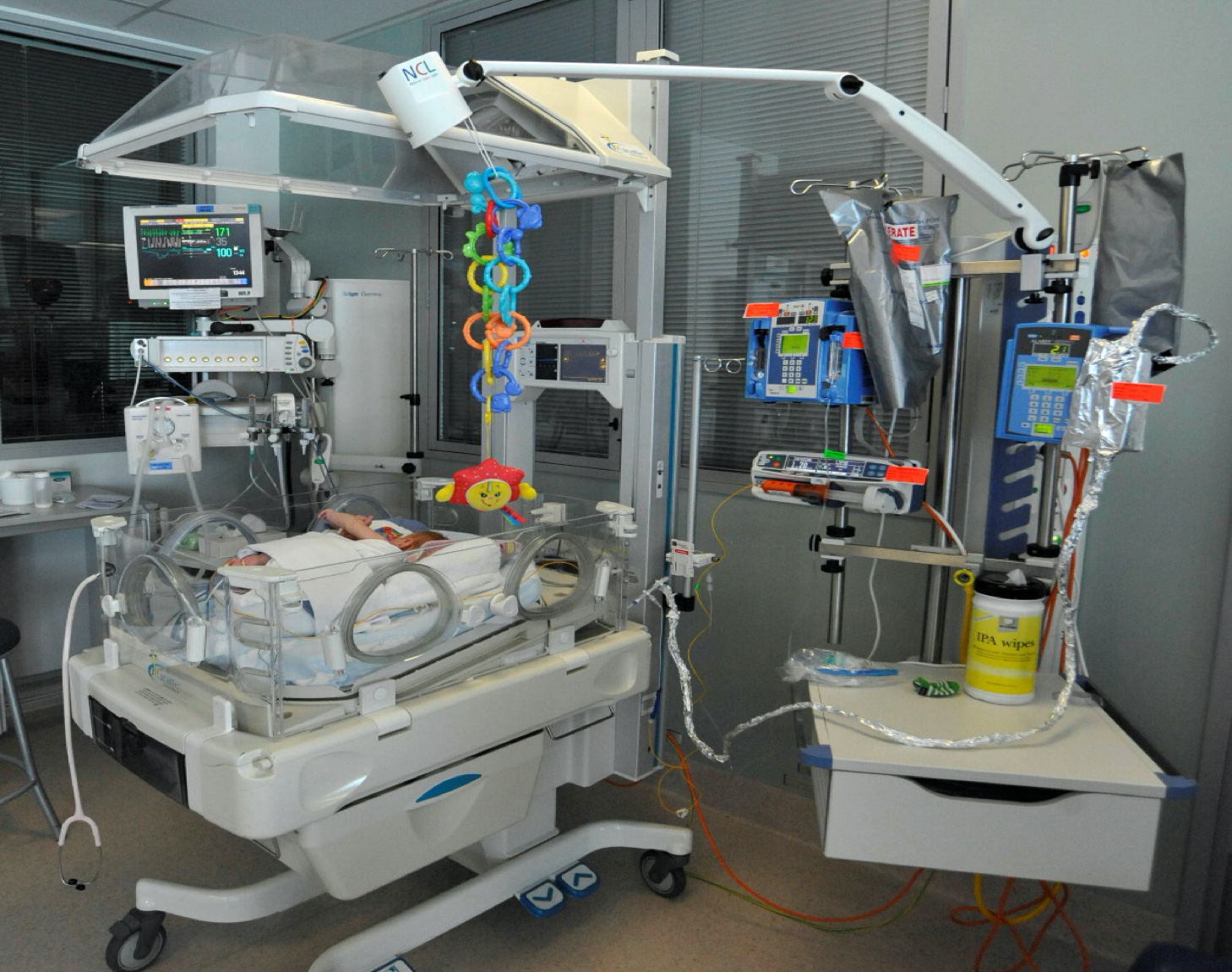
The new NICU opened in 2008
Vaughan Richardson retired in 2021. Callum Gately was appointed the new Clinical Leader, NICU.
Thanks go to Rosemary Escott and Vaughan Richardson for much of the above story and photographs.
top of page